Research Snapshot: Communication Tools to Support Public Understanding and Awareness of COVID-19 Information
What is this research about?
This article details the COVID-19 Printables project, which produced accessible, evidence-based communication tools for COVID-19 specifically aimed at vulnerable populations such as refugees, immigrants, and communities with lower literacy levels. The publication documents the project’s participatory design process and its approach to rapidly developing and adapting health information resources for these groups during the pandemic.
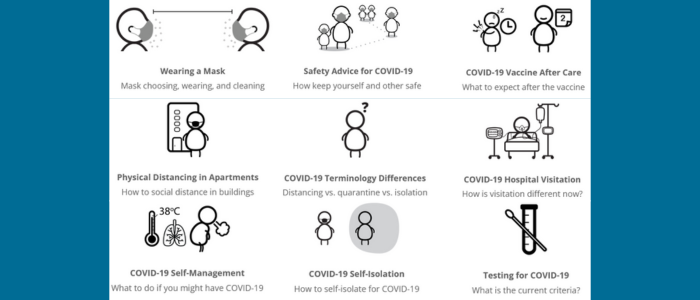
The COVID-19 Printables project created nine open-access, easy-to-use, single-page printable documents available online in over 40 languages. They were widely adopted in emergency departments, immigrant and refugee services, and community health centres in Canada and globally.
Guiding questions addressed in this article:
- How can health information during a crisis situation like COVID-19, be delivered quickly, clearly, and inclusively during a pandemic?
- Which design features (icons, plain language, and multilingual formats) most effectively improve comprehension for low-literacy and non-English-speaking groups?
- What barriers and facilitators affect the uptake of such tools by front-line health providers and community organizations?
The COVID-19 Printables project demonstrates the power of rapid, participatory, visual health communication tailored to underserved populations, setting a new precedent for scalable, inclusive public health messaging. Its approach, outcomes, and lessons offer actionable guidance for healthcare providers, policymakers, community organizations, and researchers facing current and future health crises.
What do you need to know?
The Printables project was launched in response to urgent communication gaps at the outset of the COVID-19 pandemic. Existing health information was often overly text-heavy, inaccessible for people with low literacy, and unavailable in many languages. This issue was particularly pronounced among refugees and immigrants who also faced structural and cultural barriers to healthcare information.
Key Contextual Points:
- Health-literacy research suggests that visual, icon-rich materials improve comprehension for audiences lacking advanced literacy.
- Vulnerable groups often lack digital access, which necessitated printable, offline-ready formats suitable for distribution in clinics, shelters, and emergency departments.
- The project used a community-first, participatory approach, involving clinicians, community members, and translators from the outset to ensure relevance and trust. Rapid co-design, iterative testing, and inclusivity were central to the strategy.
- Materials were intentionally designed to be welcoming and easy to disseminate.
- The Printables collection is notable for being large-scale, multilingual, openly licensed (using Creative Commons licensing), and easily editable for local adaptation. It created a model for rapidly deployed, community centred, scalable communication assets in future health crises.
What did the researchers find?
Nine evidence-based documents were developed, translated into more than 40 languages that reached over 40,000 people in Canada, with broader global impact. Their rapid approach filled crucial gaps in languages not covered by official sources, such as Rohingya and Kurdish, targeting particularly vulnerable communities.
Key Findings:
- High Usability and Preference: Survey respondents praised the materials’ clarity, brevity, visual icons, and accessibility across multiple languages. One respondent indicated these were the reasons to “choose the Printables over another resource.”
- Visual Communication Efficacy: Visual, icon-based methods worked well for low-literacy, multilingual audiences. However, not every health concept could be conveyed through icons alone. Supporting text was sometimes necessary for complex ideas.
- Iterative Improvement: Icon comprehension testing led to refinements, while analytics and user feedback determined which languages and topics to prioritize.
- Rapid Uptake: Availability and quick access were critical to practical use. One participant stated they “used whatever I could find on the day – if something was printed and available in my area, I used that over something I had to search for.”
- Mixed Comprehension Results: Most participants found the printables self-explanatory. Some icons required adjustments and additional text, especially for complex health messages.
- Barriers to Use: Some health professionals indicated their organizations had concerns about risk management because the printables were not issued by an official public health agency, despite major endorsements.
- Scalability Beyond Initial Target: The printables rapidly expanded from their original use in hospital emergency departments to community and newcomer health networks. Social media and professional connections played major roles in this organic spread.
How can you use this research?
The authors propose future randomized studies to rigorously evaluate the Printables’ impact compared to conventional, text-heavy resources. They recommend community health and newcomer-serving organizations strengthen partnerships and capacity to continue advancing health literacy and communication equity.
For Healthcare Organizations and Emergency Departments:
- Rapidly implement visual, multilingual communication tools that can be printed and distributed to patients.
- Prioritize accessibility and speed over institutional branding, especially during emergencies.
- Partner with community organizations to ensure materials reach groups most in need.
For Public Health Agencies:
- Make visual-first, inclusive communication the default in guidance, especially for emerging health crises.
- Use participatory design methods, bringing community members into the design process from the beginning.
- Create flexible templates that can be quickly updated and adapted locally.
- Invest in multilingual and visual resources before an emergency arises.
For Community Organizations Serving Immigrants and Refugees:
- Advocate for culturally sensitive and linguistically appropriate health communication.
- Build capacity to translate and adapt materials quickly as situations evolve.
- Establish networks to share and disseminate resources efficiently.
For Researchers and Academics:
- Consider a formal evaluation of visual communication tools’ effectiveness through randomized controlled trials comparing traditional materials and the Printables.
- Further research can strengthen evidence on impacts for health behaviors, information retention, and outcomes among different groups.
Further reading
Authors: Christina Derya, Christopher Rice, Maryam Mallakin, Alessandra Ceccacci, Sahil Gupta, Samuel Vaillancourt, Akm Alamgir and Kate Sellen.
Publication: Design for Health.
Related Access Alliance Activities
Client Perspectives on the Impacts of COVID-19
Recognizing the significant changes and challenges facing the centre and our community a year into the COVID-19 pandemic in Toronto, Access Alliance initiated a strategic planning process in the spring of 2021. To fully understand the situation, we needed to engage directly with our service-users. We conducted seven virtual focus groups between April 8 and 21, 2021 (using the Zoom platform). A total of 64 community members took part, including people of various genders, ages, education levels, sexual orientations, and cultural backgrounds.
Vaccine Engagement Impact Report
Taylor Massey-Oakridge-Victoria Village was one of the least vaccinated neighbourhoods during the summer/fall of 2021. With a coordinated effort between the partners, we raised the vaccination rate above the City’s average and significantly reduced the COVID-19 hospitalization rates during the pandemic peak.
Vaccine hesitancy among Syrian refugee parents in Canada: A multifaceted challenge in public health
This multi-country multi-institute study, housed at Access Alliance, investigates vaccine hesitancy among Syrian refugee parents in Canada. Researchers examined the factors that influence their willingness to accept COVID-19 vaccination.
